Cold Chain & Vaccine Logistics, Built for Product Integrity, Field Readiness, and Supply Continuity
Cold chain and vaccine logistics is often treated as a downstream operational function, something that begins only after manufacturing has ended. In practice, that view is too narrow. Cold chain and vaccine logistics begins much earlier, at the point where a product’s thermal profile, presentation format, stability window, and deployment pathway start to shape one another. At Elise Biopharma, cold chain and vaccine logistics is not treated as a handoff. It is treated as part of the product system itself.
For vaccines, biologics, and advanced sterile products, cold chain and vaccine logistics can quietly determine whether a programme remains viable at scale. A process may perform well in development. Fill-finish may be executed correctly. Release data may look clean. Yet if the product cannot tolerate real transport conditions, real storage variability, real in-use handling, or real clinic workflows, the operational model begins to fray. This is why cold chain and vaccine logistics must be designed with as much seriousness as upstream process development or sterile manufacturing.

At Elise Biopharma, cold chain and vaccine logistics is approached as a discipline that links formulation, presentation, storage, transport, in-use policy, packaging, and release strategy into a coherent supply framework. That is especially important for products moving through demanding conditions: vaccines distributed across regions with uneven infrastructure, sterile injectables requiring temperature-sensitive handling, lyophilised products that still depend on controlled post-fill logistics, and biologics where temperature drift can alter potency, particle behaviour, aggregation, or shelf-life.
Cold chain and vaccine logistics should not feel like a courier problem. It should feel like part of the programme architecture. That is the approach we take.
Why Cold Chain & Vaccine Logistics Matters
Cold chain and vaccine logistics is one of the most overlooked determinants of success in vaccine programmes and sterile biologic supply. The reason is simple: many problems do not appear until the product has already left the manufacturing environment.
A batch that is technically within specification can still become operationally fragile if the temperature pathway, packaging logic, or in-use conditions were not designed around how the product will actually move.
Cold chain and vaccine logistics matters because it governs:
- temperature control across shipment and storage
- product stability in real transit conditions
- handling windows at clinics, hospitals, and field sites
- final presentation compatibility with deployment settings
- shelf-life interpretation under practical use conditions
- the resilience of supply during scale-up or geographic expansion
For vaccine programmes especially, cold chain and vaccine logistics often becomes the hidden bridge between manufacturing readiness and public health usability. A product that requires overly rigid handling, unclear thawing rules, impractical beyond-use timing, or expensive distribution conditions may create friction at exactly the stage where the programme needs adoption and reliability.
At Elise Biopharma, cold chain and vaccine logistics is built to minimise that friction. The goal is not just to preserve the product chemically. The goal is to preserve its operational integrity all the way to the point of use.
Core Cold Chain & Vaccine Logistics Capabilities
Our cold chain and vaccine logistics capabilities are designed to support temperature-sensitive programmes from manufacturing release through deployment readiness.
Storage Strategy
- frozen, refrigerated, and controlled-temperature product pathways
- stability-informed storage condition selection
- short-term and long-term storage planning
- alignment of temperature profiles with product-specific risk
Transport Readiness
- shipping lane assessment and packaging logic
- excursion-aware distribution planning
- thermal packaging strategy
- transfer conditions matched to product sensitivity
In-Use Handling Design
- thawing and hold-time guidance
- draw-up and puncture-use windows
- clinical and pharmacy workflow fit
- beyond-use policy design grounded in actual product data
Presentation and Deployment Alignment
- vial, syringe, and cartridge logic linked to logistics burden
- packaging decisions that support stability and usability
- field-ready presentation assessment
- route-to-patient realism built into supply planning
Programme Continuity
- lot sequencing and storage planning
- release timing linked to deployment pathways
- coordination with fill-finish and commercial supply
- logistics continuity across early, regional, and expanded supply models
Cold chain and vaccine logistics only works when storage, transport, and use conditions are considered together. A product that is stable in storage but vulnerable during thaw, puncture, transport, or draw-up is not truly logistics-ready.
Logistics for Vaccines and Sterile Biologics
Vaccines and advanced biologics do not fail loudly. More often, they drift—subtly, incrementally—through mechanisms that only become visible when performance no longer matches expectation. Protein aggregation shifts by a few percentage points. Lipid nanoparticle size distribution broadens. RNA integrity degrades along a non-linear curve tied to thermal exposure history rather than a single event.
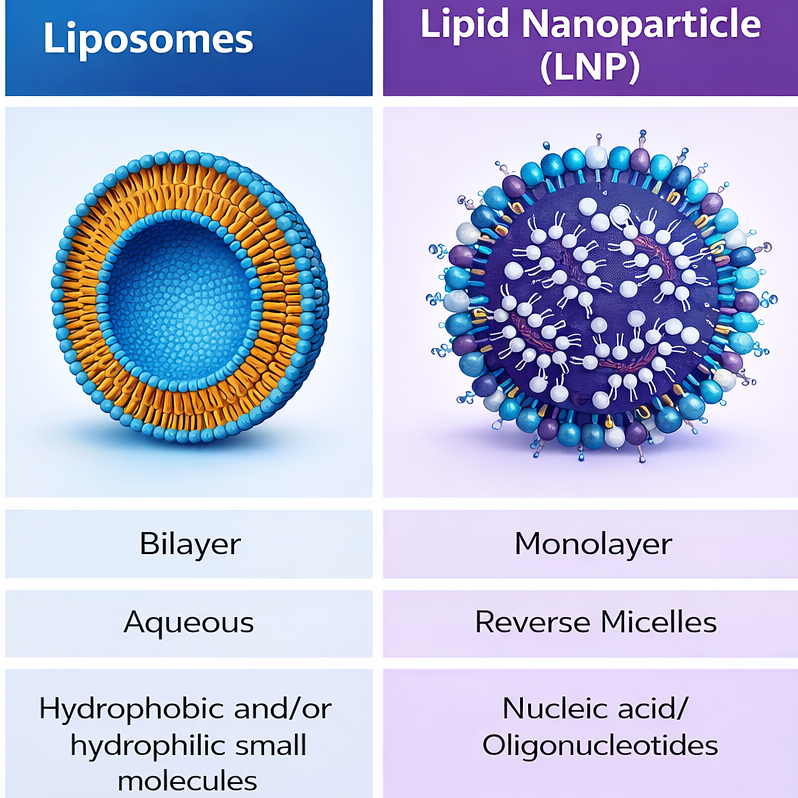
This is why cold chain and vaccine logistics cannot be reduced to storage labels or nominal temperature bands. The system must reflect molecular behaviour under transit conditions, not just compliance ranges.
Sensitive modalities introduce different failure modes:
- viral vectors influenced by shear-induced capsid disruption and freeze-thaw cycling
- recombinant proteins susceptible to interfacial adsorption and aggregation nucleation
- mRNA systems governed by hydrolysis kinetics and lipid phase transition thresholds
- adjuvanted formulations where emulsion stability and droplet coalescence shift under thermal stress
- high-concentration biologics exhibiting viscosity-dependent diffusion and phase separation effects
Each of these responds differently to temperature excursions, agitation, and time-at-condition. A product stored at 2–8°C is not necessarily stable at 2–8°C in motion, or after multiple transitions across that range.
What matters is not the label claim—it is the thermal history profile.
Effective cold chain and vaccine logistics therefore maps what the product actually experiences:
- pre-shipment staging where dwell time introduces thermal lag and gradient formation
- transport phases with micro-excursions that fall within range but accumulate impact
- cross-docking events that introduce uncontrolled ambient exposure windows
- cold room entry/exit cycles where condensation and rapid equilibration occur
- thawing kinetics influenced by container geometry and fill volume
- in-clinic handling where timing, agitation, and repeated access redefine stability conditions
A useful but underutilised concept here is mean kinetic temperature (MKT)—not as a regulatory checkbox, but as a modelling tool for cumulative thermal stress. Many systems meet excursion criteria while still exceeding meaningful MKT thresholds over time.
At Elise Biopharma, logistics design begins with product behaviour curves rather than standard templates. Stability is treated as a dynamic system, not a fixed boundary.
Temperature Excursions, Stability Windows, and Real-World Use
Excursions are often framed as binary events: acceptable or unacceptable. In reality, they are probabilistic. The same deviation may be negligible for one product and structurally damaging for another.
The critical variable is not the excursion itself, but the interaction between temperature, time, and formulation sensitivity.
Within cold chain and vaccine logistics, this leads to more nuanced control strategies:
- excursion frameworks based on Arrhenius-derived degradation models, not fixed-duration assumptions
- stability windows defined by time-temperature integrals rather than static limits
- post-thaw usability linked to glass transition temperature (Tg’) recovery behaviour
- reconstitution timing informed by osmotic balance and solubilisation kinetics
- packaging selection based on thermal conductivity and phase change buffering capacity
One recurring issue: short, repeated deviations often have more impact than a single longer event. This is especially true in systems sensitive to thermal cycling-induced stress, where repeated expansion and contraction affect structure over time.
Another overlooked factor is in-use degradation acceleration. Once a vial is punctured or a product is reconstituted, it transitions into a different kinetic regime—often governed by oxidation, microbial ingress risk, or surface adsorption.
Elise Biopharma structures policies around these realities:
- excursion response protocols tied to actual degradation pathways
- in-use limits that reflect post-access stability, not unopened container data
- thaw and reconstitution guidance based on empirical handling studies
- packaging configurations aligned with known vulnerability points
The result is a system that manages excursions rather than overreacting to them—reducing unnecessary product loss while maintaining control.
Packaging Strategy and Distribution Design
Packaging is often treated as a passive layer. In practice, it is an active control system.
Thermal performance, mechanical protection, dose density, and usability are all functions of packaging design. A poorly selected configuration can negate otherwise robust stability data.
Within cold chain and vaccine logistics, packaging decisions influence:
- heat transfer rates governed by insulation R-value and phase change material (PCM) behaviour
- internal temperature uniformity affected by load configuration and void space distribution
- breakage risk tied to shock absorption coefficients and container geometry
- storage density driven by secondary packaging footprint and palletisation logic
- last-mile usability shaped by carton access design and dose presentation format
A niche but impactful variable is thermal mass distribution. Uneven loading within a shipper can create localised hot or cold spots, even when average temperatures remain compliant.
Similarly, re-icing cycles introduce variability that is rarely modelled accurately. Each cycle changes the internal thermal profile, particularly if PCM conditioning is inconsistent.
At programme level, packaging becomes a lever for operational efficiency:
- increasing doses per shipper reduces cost but may increase thermal recovery time after opening
- smaller configurations improve flexibility but reduce temperature buffering capacity
- multi-dose formats optimise distribution but introduce in-use stability complexity
Elise Biopharma integrates packaging into early planning, treating it as part of the product system rather than a downstream procurement decision.
Clinical, Commercial, and Public Health Deployment
Logistics systems evolve as programmes scale, but failure often occurs when each phase is treated as a reset rather than a progression.
Clinical supply emphasises control:
- tightly defined shipment lanes
- site-specific storage mapping
- controlled thaw and handling instructions
- full chain-of-custody visibility
Commercial supply introduces rhythm:
- synchronisation between manufacturing cadence and distribution cycles
- inventory strategies linked to expiry dating and release timing variability
- standardised packaging for repeatability across markets
Public health deployment introduces variability:
- infrastructure heterogeneity across regions
- intermittent power stability affecting cold storage reliability
- handling by non-specialist personnel
- expanded exposure to environmental fluctuation
In this phase, cold chain and vaccine logistics becomes less about precision and more about tolerance. Systems must function even when conditions degrade.
A practical insight: the most robust programmes simplify as they scale. Not by reducing scientific rigor, but by reducing operational fragility—fewer steps, clearer instructions, more forgiving handling windows.
Interested in a discussion? Contact us today!
Fill-Finish Integration and Downstream Impact
Logistics does not begin after manufacturing. It is encoded into the product at fill-finish.
Container selection alone can shift the entire distribution profile:
- vial formats influence headspace gas composition and oxidation risk
- prefilled syringes alter surface interaction dynamics and dose accuracy constraints
- cartridge systems introduce device compatibility and pressure tolerance considerations
Volume and concentration affect:
- freeze and thaw rates through thermal mass scaling
- viscosity-dependent handling during administration
- dose extraction efficiency in multi-dose settings
Closure systems determine:
- seal integrity under transport stress
- oxygen ingress rates
- puncture performance over repeated access
A recurring misalignment in many programmes is treating presentation as interchangeable. In reality, each format defines a different logistics pathway.
Niche Operational Factors That Quietly Matter
The stability of a logistics system is often decided by small, cumulative variables:
- thaw protocols that vary between operators, altering temperature ramp rates
- agitation sensitivity during transport leading to protein unfolding or nanoparticle disruption
- condensation affecting label integrity and traceability
- draw-up timing influencing dose accuracy in viscous formulations
- pallet configuration impacting airflow and temperature distribution
- customs delays introducing unplanned ambient exposure intervals
- clinic workflows that unintentionally extend in-use time
These are not edge cases. They are routine conditions.
Strong cold chain and vaccine logistics anticipates them—designing instructions, packaging, and processes that reduce dependency on perfect execution.
At Elise Biopharma, this layer of detail is treated as part of system design, not post-deviation analysis.
Data, Documentation, and Supply Confidence
A logistics system is only as reliable as the clarity of its data.
Temperature limits, excursion policies, and handling instructions must be both scientifically grounded and operationally usable. Ambiguity at this level propagates quickly across distribution networks.
Effective systems support:
- storage and transport claims backed by stability-indicating methods
- clearly defined in-use and beyond-use dating
- excursion decision trees aligned with degradation mechanisms
- concise, field-ready handling instructions
- quality review frameworks for logistics events
When multiple regions, partners, and stakeholders are involved, documentation becomes a control mechanism—not just a record.

The outcome is not just product protection. It is confidence across the supply chain, where decisions are consistent, defensible, and repeatable.
Why Teams Choose Elise Biopharma for Cold Chain & Vaccine Logistics
Organisations do not usually seek cold chain and vaccine logistics support because they want abstract advice. They seek it because they know the product must survive the journey as well as the process.
Teams choose Elise Biopharma because our cold chain and vaccine logistics approach:
- begins early in the programme
- connects directly to manufacturing and fill-finish
- accounts for actual product sensitivity
- supports real deployment pathways rather than idealised ones
- balances technical quality with practical field use
This matters for vaccine developers, biologics sponsors, animal health programmes, advanced sterile products, and any organisation trying to avoid the costly gap between product release and product usability.
A Better Standard for Logistics-Ready Product Design
The strongest cold chain and vaccine logistics systems do not merely preserve product. They reduce avoidable complexity.
They create:
- clearer storage pathways
- more realistic in-use policies
- better field handling
- fewer preventable excursions
- more durable supply continuity
- stronger alignment between product science and real deployment
That is the standard Elise Biopharma works to.
Our cold chain and vaccine logistics model is built for:
- vaccines requiring controlled temperature pathways
- biologics with meaningful thermal sensitivity
- sterile products needing integrated presentation and logistics planning
- programmes that must move from release into real-world use without operational erosion
When cold chain and vaccine logistics is done correctly, the product reaches the point of use in the condition it was designed to be in, with instructions that make sense and a supply chain that can actually sustain the programme.
Cold Chain & Vaccine Logistics That Actually Holds Up
Cold chain and vaccine logistics is where good science either survives contact with reality—or doesn’t. It’s not just about staying within range. It’s about whether the product still behaves the way it should after being moved, handled, opened, and used.
At Elise Biopharma, cold chain and vaccine logistics is built into the system early. Storage logic, transport design, fill-finish decisions, and in-use handling all connect—so the product doesn’t lose integrity somewhere between the line and the clinic.
For teams building modern vaccines and biologics, that connection matters. It’s the difference between something that works on paper and something that works in the field.
Email our team at: info@elisebiopharma.com
